Stress Reactivity Laboratory Procedures
PCS3 included two laboratory acute stress-reactivity and recovery sessions designed to evaluate psychological, cardiovascular and cortisol responses to a laboratory challenge task. Both sessions were conducted between the hours of 3 p.m. and 9 p.m., to control for diurnal variations in cortisol. Each session took place at the University of Pittsburgh and lasted about 21/4 hours. Session 1 took place 2-4 weeks prior to viral challenge, and session 2 took place 4-6 weeks post-challenge.
Protocol
For each session, participants were asked to abstain from alcohol for 48 hours, from exercise (above that required in one's usual daily schedule) and non-prescription medications for 24 hours, from eating and drinking (except water) for 2 hours, and from smoking for 1 hour prior to the session. Participants were advised to continue any medication prescribed by a medical doctor. Upon arrival at the laboratory, participants were interviewed by the session coordinator to determine whether they had followed the pre-session instructions (see pre-session interview form), and then asked to provide a saliva sample for measurement of cortisol (see Salivary Cortisol Sample Collection). Also at this time, participant height, weight, and waist and hip circumferences were measured (see Anthropomorphic Measures), and resting blood pressure (BP) taken.
After entering the experimental chamber, participants were instrumented with an automated blood pressure (BP) cuff for measurement of systolic and diastolic blood pressure (SBP and DBP), mean arterial pressure (MAP), and heart rate (HR); three electrocardiogram (ECG) leads for measurement of heart rate variability (HRV); and a respiration belt for assessment of breathing rate. While participants were in the standing position, three ECG electrodes were placed on the chest using a modified lead II configuration (i.e., one at the right mid-clavicular line directly below the clavicle; and one each at the left and right lower margins of the ribcage in line with the midpoints of the respective left and right clavicles), and the respiration monitoring belt (used with gas pressure sensor; Vernier Software & Technology, Beaverton, OR) fitted loosely around the thorax. Participants were then seated in a reclining chair set in the upright position; the respiration belt was inflated until snug but not restricting participant breathing; and an automated BP cuff1 (Critikon Dynamap® Vital Signs Monitor 1846SX, GE Healthcare, U.S.) was placed on the non-dominant arm (see Figure).
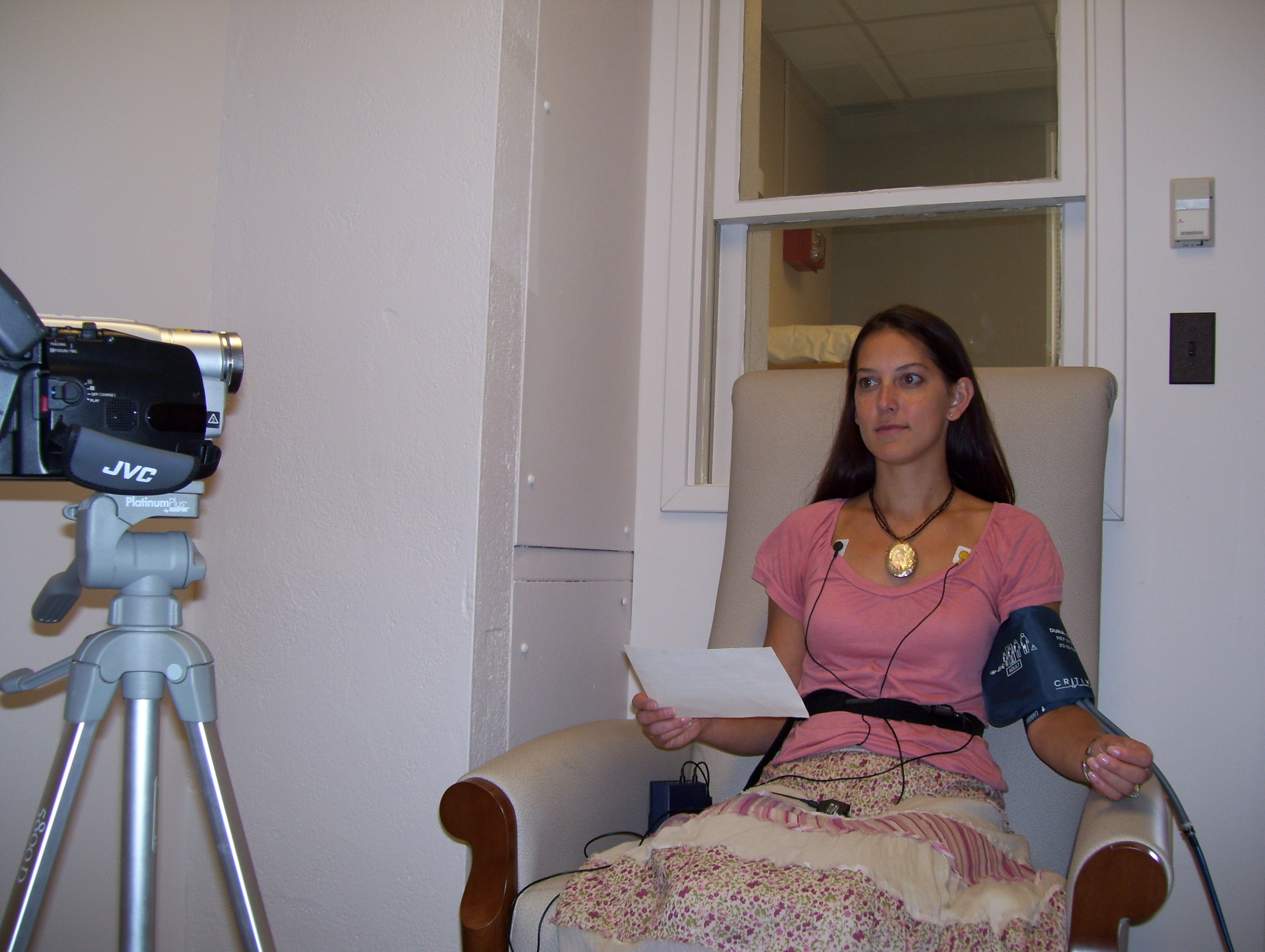
Figure 1. Participant instrumented with physiologic recording equipment during speech delivery phase of the laboratory stress reactivity protocol.
Baseline Period
Following instrumentation, participants sat quietly for a 20 minute baseline (habituation) period. HRV and respiration were recorded throughout this period, and HR and BP were measured 4 times (every 120 seconds) during the last 6 minutes. At minute 20, a second saliva sample for measurement of cortisol was collected. Immediately following the baseline period, participants completed a self-administered stress-reactivity questionnaire (SRQ) that assessed levels of state positive and negative mood during the baseline period (see Figure 2).
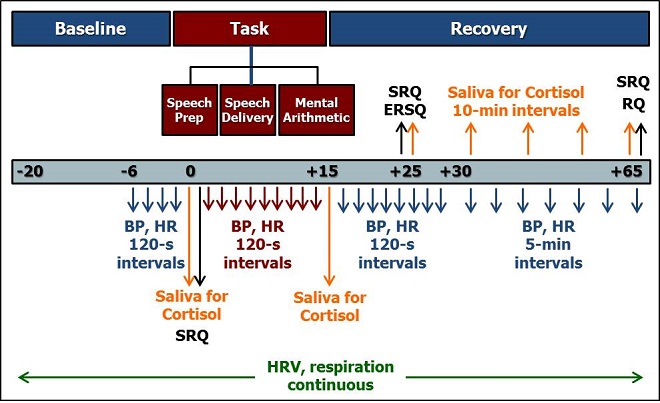
Figure 2. Laboratory stress reactivity protocol. SRQ = Stress Reactivity Questionnaire.
ERSQ = Emotional Response to Stress Questionnaire. RQ = Rumination Questionnaire.
Task Period
Following the baseline, participants completed a modified version of the Trier Social Stress Test (TSST)2, a well-validated and widely used acute stress protocol that lasts 15 minutes and involves a simulated public speaking task followed by a mental arithmetic task. For the public-speaking task, participants were given 5 minutes to prepare a speech defending themselves against an alleged transgression (shoplifting or traffic violation counterbalanced across the two occasions of testing), followed by 5 minutes of videotaped speech delivery. Participants were told that their speech was being evaluated. At the end of the speech task, a second experimenter (the “evaluator”) entered the chamber and provided the instructions for the mental arithmetic task which were comprised of asking the participant to serially subtract the number 13 from 1,022 as quickly and as accurately as possible. The evaluator remained in the chamber while participants performed the task, and instructed participants to restart the task any time that they made a subtraction error. (During the second stress reactivity session, participants were asked to subtract the number 13 from 1,039 in the presence of a different evaluator). The mental arithmetic task lasted for 5 minutes. HR and BP were recorded every 120 seconds and HRV and respiration continuously throughout the task period. A third saliva sample was collected immediately following the task period (see Figure 2).
Recovery Period
After the task, participants were instructed to rest quietly for a 50-minute recovery period. During this period, BP and HR were measured every 120 seconds for the first 15 minutes (8 readings) and then every 5 minutes (7 readings). HRV and respiration were measured continuously for the first 10 minutes of the recovery period. Saliva for cortisol measurement was collected every 10 minutes throughout this period (5 samples). Ten minutes after the start of the recovery period participants again completed the SRQ, this time reporting on state mood during the task component of the protocol. Participants also completed a second self-administered questionnaire that assessed emotional response to the task (ERSQ). At the end of the recovery period, participants completed the SRQ a third time to assess state mood during that component of the protocol, as well as a questionnaire assessing the degree of rumination about the task and any other negative thoughts that may have occurred to them during the recovery period (see Figure 2).
1The Critikon Dynamap® Vital Signs Monitor 8100 was used for a small number of participants (<10) in the final cohort of PCS3.
Reference
2 Kirschbaum, C., Pirke, K.-M., & Hellhammer, D. H. (1993). The ‘Trier Social Stress Test’ – A tool for investigating psychobiological stress responses in a laboratory setting. Neuropsychobiology, 28, 76-81.