Researchers Discover What Pneumococcus "Says" to Make You Sick
Carnegie Mellon University researchers have identified a molecule that plays a key role in bacterial communication and infection. Their findings add a new word to pneumococcus' molecular dictionary and may lead to novel ways to manipulate the bacteria and prevent infection. The findings, from the lab of Associate Professor of Biological Sciences Luisa Hiller, are published in the Oct. 11 issue of PLOS Pathogens.
Organisms worldwide communicate in their own unique ways: humans use words, bees dance and fireflies glow. Decoding a community's common language provides the ability to understand and influence the community's behavior.
What if bacteria also have their own language? By understanding that syntax, could we simply ask the bacteria to stop making us sick?
These questions are at the core of Hiller's research. Her lab is investigating "bacterial linguistics," attempting to identify the "words" that bacteria use to communicate. They hope to assemble a dictionary that will give researchers the vocabulary they need to manipulate deadly pathogens.
The Hiller lab is unraveling how bacterial communication contributes to disease and antibiotic resistance, focusing on the bacterium pneumococcus.
Pneumococcus frequently colonizes children and the elderly. It can inhabit the back of the throat without causing any symptoms, but when it spreads to tissues beyond the throat, it can cause mild to severe disease. Pneumococcus is the leading cause of upper respiratory disease and a common cause of pneumonia and pediatric ear infections. Worldwide, it is responsible for more than one million deaths each year.
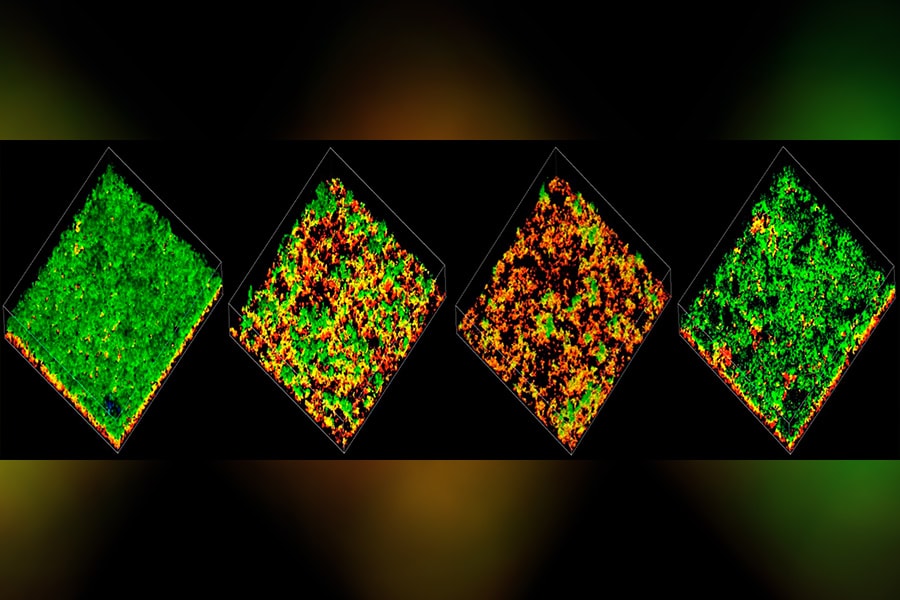
Pneumococcus forms and thrives in communities called biofilms. The community provides an environment where cells communicate, cooperate and battle. The biofilm also protects the bacteria from antimicrobial interventions and serves as a breeding ground for antibiotic resistance.
In the biofilm, pneumococcus secretes many molecules that appear to be used for communication — telling cells to migrate, multiply and adapt. Despite their potential role in the spread of disease, much about these molecular words is a mystery.
"If we know the meaning of bacterial words, maybe we can remove them from the system or manipulate them so pneumococcus doesn't become pathogenic," Hiller said.
In the PLOS Pathogens study, Biological Sciences graduate student Surya Aggarwal identified a previously uncharacterized pneumococcal molecule — a new word — he named BriC. He and his colleagues in the Hiller lab found BriC plays a critical role in biofilm development by signaling to bacteria to produce more biofilm during competence, a metabolic state that makes multiple cellular functions, including DNA exchange, possible. BriC is researchers' first clue to understanding how cells in competence interact with other cells to organize themselves into a biofilm.
The study authors also found that in the context of disease, BriC appears to make pneumococcal infections more robust.
"Cells growing within a biofilm are highly recalcitrant to antibiotic treatment" Aggarwal said. "Given this link, BriC assumes greater significance. It could possibly be a target to render bacteria more sensitive to antibiotic treatment."
In a final twist, the researchers also found that bacteria may also be making semantic changes to their words. They determined that some critically important clinical strains evolved a modification to produce BriC outside of competence. They also produced more BriC, and produced it more often, which enhanced biofilms. The researchers are currently investigating what this variation could mean to the development of disease in children.
"We're at the very beginning of the dictionary," Hiller said. "We will continue to dig into the meaning of BriC, and related bacterial words, as a means to manipulate bacterial language and control disease."
Additional study authors include: Rory Eutsey, Jacob West-Roberts, Wenjie Xu and Aaron Mitchell from Carnegie Mellon; Arnau Domenech and Jan-Willem Veening from the University of Lausanne; Iman Tajer Abdullah and Hasan Yesilkaya from the University of Leicester and University of Kirkuk; and Hasan Yesilkaya from the University of Leicester. Hiller is also a member of the Center for Excellence in Biofilm Research at the Allegheny Health Network.
The research was funded by the National Institutes of Health (DC-011322), the Stupakoff Scientific Achievement Award and Department of Biological Sciences at Carnegie Mellon.