New Technique Reduces Side Effects, Improves Delivery of Chemotherapy Nanodrugs
Carnegie Mellon University researchers have developed a new method for delivering chemotherapy nanodrugs that increases their bioavailability and reduces side effects.
Their study, published online in Scientific Reports, shows that administering an FDA-approved nutrition source prior to chemotherapy can reduce the amount of the toxic drugs that settle in the spleen, liver and kidneys.
Nanodrugs — drugs attached to tiny biocompatible particles — show great promise in the treatment of a number of diseases, including cancer. Delivery of these drugs, however, is not very efficient — only about 0.7 percent of chemotherapy nanodrugs reach their target tumor cells. The remainder are absorbed by other cells, including those in the liver, spleen and kidneys. When the drugs build up in these organs, they cause toxicity and side-effects that negatively impact a patient's quality of life.
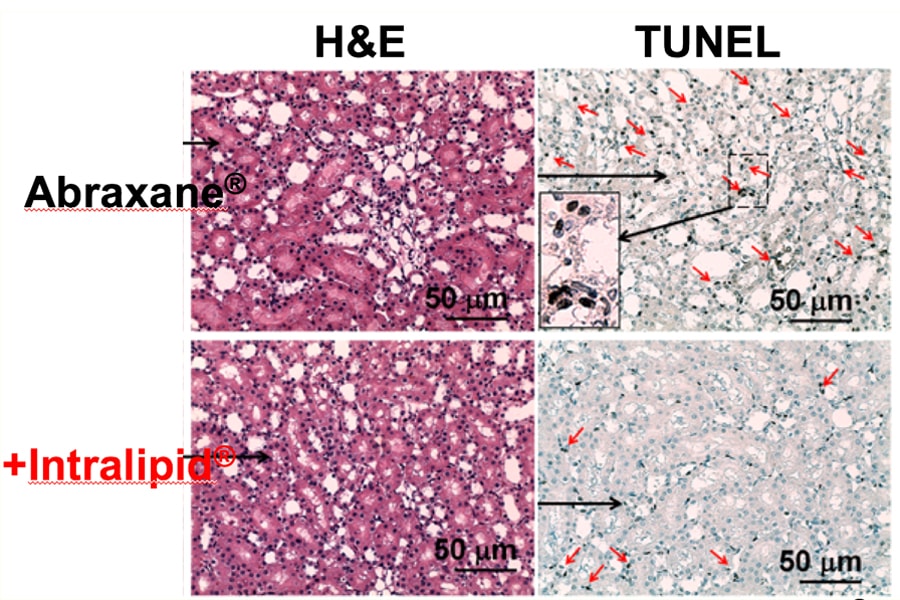
Administering a combination of Abraxane® and Intralipid® results in less toxicity of the chemotherapy drug in the kidneys (bottom row) than administering Abraxane® alone (top row).
Chien Ho, professor of biological sciences at Carnegie Mellon, and his colleagues have developed a novel way to improve delivery of chemotherapy nanodrugs by using Intralipid®, an FDA-approved nutrition source to temporarily blunt the reticuloendothelial system — a network of cells and tissues found throughout the body, including in the blood, lymph nodes, spleen and liver, that play an important role in the immune system.
Ho and colleagues tested their technique in a rat model of cancer using three FDA-approved chemotherapy nanodrugs, Abraxane®, Marqibo® and Onivyde®, and one experimental platinum-based anti-cancer nanodrug. In the study, they administered Intralipid one hour before giving the animal a chemotherapy nanodrug. They found their method reduced the amount of the drug found in the liver, spleen and kidneys and reduced the drugs' toxic side-effects. They also found more of the drug was available to attack tumor cells. Additionally, the Intralipid treatment had no harmful impact on tumor growth or drug efficacy.
The researchers believe their drug delivery methodology can be applied to a variety of nanodrugs without any modifications to the drugs.
"This methodology could have a major impact in the delivery of nanodrugs not only for patients undergoing chemotherapy for cancer treatment but also to those being treated with nanodrugs for other conditions," Ho said.