Social Integration and Health:
The Case of the Common Cold
Sheldon Cohen and Ian Brissette
Carnegie Mellon University
David P. Skoner and William J. Doyle
Children’s Hospital of Pittsburgh and the University of Pittsburgh School of Medicine
[This research
reported in this article was supported by a grant from the National
Institute of Mental Health (MH50429), a Senior Scientist Award to Dr.
Cohen from the National Institute of Mental Health (MH00721), and a
grant from the National Institute of Health to the University of
Pittsburgh Medical Center General Clinical Research Center (NCRR/GCRC
M01 RR00056). Ian Brissette’s participation was supported by Training
grant in Health Psychology from the National Institute of Mental Health
(MH19953). This interdisciplinary collaboration was facilitated by the
Pittsburgh Mind-Body Center (HL65111 & HL65112).]
ABSTRACT: In this article, we discuss the concept of social integration and its implications for health. We provide both an overview of the social epidemiology and a review of theories of how participation in a diverse social network might influence health. We also present evidence from a prospective study of social network diversity (number of social roles) and susceptibility to the common cold in people experimentally exposed to a cold virus. We found that the greater the social diversity, the lesser the susceptibility to infectious illness. However, our attempts to isolate the pathways through which social diversity was associated with susceptibility (health practices, hormones, immune function) were unsuccessful. The relation was independent of the number of people in the social network, and of personality characteristics thought to influence social participation.
Introduction
Social integration refers to the extent to which one participates in the social community. Those studying social participation and health have treated social integration as a characteristic of individuals rather than a characteristic of communities. Consequently, measures of social integration in this literature are based on individual self-reports of the numbers and types of social relationships, the extent of participation in social activities, or the perception of being an integrated member of the community (see review in Brissette, Cohen & Seeman, 2000).
Prospective community studies indicate that greater levels of social integration are associated with lower rates of mortality (reviewed by Berkman, 1995) and fewer depressive symptoms (reviewed by Cohen & Wills, 1985). Similarly, studies of patient populations find that social integration is associated with a greater likelihood of survival following a heart attack (reviewed by Berkman, 1995), and lesser likelihood of suffering a recurrence of cancer (reviewed by Helgeson, Cohen & Fritz, 1998). The magnitude of the health risk of being relatively isolated is comparable to the risks associated with cigarette smoking, high blood pressure and obesity and is robust even after controlling for these and other traditional risk factors (House et al., 1988; Orth-Gomer & Johnson, 1987).
Social Integration Theories
The concept of social integration is rooted in Durkheim’s (1897/1951) seminal work on social conditions and suicide. He proposed that stable social structure and widely held norms are protective and regulate behavior. Consistent with this reasoning was his observation that suicide was most prevalent among individuals who were not married and lacked ties with the community and church.
Faris’s (1934) work on cultural isolation and the development of mental illness also emphasized the importance of social contacts (cf. Jaco, 1954; Ware, 1956). Faris (1934) suggested that socially isolated individuals were at a higher risk for mental disorder. His ideas were grounded in symbolic interactionist tradition and assumed that social interaction was essential to the development of normal personality and the enactment of appropriate social conduct.
In contrast to their predecessors, a number of sociologists later suggested that participation in multiple social domains was detrimental to psychological well-being (Goode, 1960; Slater, 1963; Coser, 1974). These theorists viewed people’s social environments as sets of interrelated role relationships (e.g., parent, husband/wife, volunteer, church member and worker). Each role required a different set of obligations with greater numbers of roles causing conflicting obligations and the concomitant experience of stress. Goode (1960) coined the term "role strain" to describe the difficulty involved in adequately performing multiple roles simultaneously. Role strain consists of two components, role conflict and role overload. Role conflict occurs when the expectations associated with different roles are discrepant. Role overload occurs when honoring expectations associated with some roles is at the expense of honoring expectations associated with others. As one accumulates more roles, the probability of experiencing role conflict and role overload increases.
Although Goode’s ideas have some intuitive appeal, the empirical data have provided only limited support (e.g., Sieber, 1974, Thoits, 1983). In contrast to Goode (1960), Sieber (1974) proposed that possessing multiple roles is beneficial for psychological well-being. He argued that rewards afforded by multiple roles exceed the burdens associated with role strain. Proposed rewards included privilege accumulation, status security, status enhancement and self-esteem enhancement. Marks (1977) also suggested that multiple roles were not burdening and added that they could be potential sources of wealth, prestige, sympathy, approval and favorable self-image. Both Sieber (1974) and Marks (1977) promoted the notion that role accumulation is more gratifying than stressing. This idea is referred to as the "role accumulation theory." Role accumulation theory resonates with Faris’s social isolation hypothesis. Both theoretical views propose that greater levels of social interaction are associated with greater well-being. However, a critical distinction can be made between the two. Whereas Faris (1934) focused on isolation as a stressor, Marks (1977) and Sieber (1974) suggest the greater and more diverse one’s social contacts the better.
A more explicit theory of how social integration benefits health and well-being was proposed by Thoits (1983). Consistent with symbolic interactionist theorists (Mead, 1934; Stryker, 1980), Thoits argued that people’s identities are tied to their social roles. Social roles are viewed as sets of behavioral expectations that emerge from the social environments in which one interacts. These behavioral expectations impose a sense of predictability in people’s lives by providing information about how one ought to act. Also, by meeting role expectations individuals are given the opportunity to enhance self-esteem.
Thoits (1983) suggested that role-identities provide people information about who they are in an existential sense. Social roles provide a purpose to life. Thus, as people accumulate role-identities the sense that they possess a meaningful, guided existence strengthens. It is implied that a sense of meaning in life is an integral component of psychological well-being and that failing to have a sense of meaning often leads to improper conduct and deviant self-destructive behavior. This position is called the "identity accumulation" hypothesis (Thoits, 1983).
We (Cohen, 1988) expressed a position similar to Thoits (1983) in our description of identity and esteem models of the psychological influence of social relationships. Specifically, we suggested that the ability to meet role expectations might result in cognitive benefits such as increased feelings of self-worth, purpose and meaning of life, and control over one’s environment, which may influence health through a variety of pathways. One benefit afforded by holding multiple social roles is the attenuation of negative affective states and generation of positive affect (Cohen, 1991). In turn, improved (more positive and less negative) affective states have been associated with changes in immune functioning that are thought to enhance one’s ability to fight off infectious agents (e.g., Cohen & Herbert, 1996; Glaser, Rabin, Chesney, Cohen & Nathanson, 1999). These changes in affect are thought to influence immunity by altering circulating levels of a number of hormones, primarily epinephrine, norepinephrine, and cortisol, that regulate immune response (Rabin, 1999). We (Cohen, 1988) also suggested that holding multiple social roles may impact health through social and informational influence. For example, integrated individuals are subject to social controls that may promote the adoption of healthful behaviors and prevent behaviors with defined health risks (cf. Umberson, 1987; Rook, 1990). Social network members may also act as sources of information regarding appropriate medical care, and provide feedback that could influence symptom reporting and compliance with medical regimens.
The Pittsburgh Common Cold Study
As a part of a larger research project on the role of psychological and behavioral factors in risk for infectious illness, we were able to address the hypothesis that holding greater numbers of social roles contributed to host resistance—the ability of the body to fight off infectious agents. We refer to the number of social roles as "network diversity" to distinguish it from other conceptualizations of social integration. Interestingly, in the natural environment, having more diverse networks probably increases the risk of upper respiratory infection. This is because viruses cause common colds and contact with a larger and more diverse group of people would increase exposure to viruses circulating in the community. However, our interest was not in exposure but rather in the body’s ability to resist infectious illness when exposed to an infectious agent. We studied host resistance by intentionally exposing our subjects to specific common cold viruses. We controlled the dose of virus they were exposed to, their previous exposure to the experimental virus (as indicated by their level of specific antibody to the virus at baseline), and their concurrent exposure to alternative infectious agents during the course of the trial (by keeping the subjects in quarantine).
The specific questions we posed were:
-
(a) Are people with more social roles (greater network diversity) less
likely to develop a clinical illness when they are experimentally
exposed to a virus? If so, is this association attributable entirely to
isolated people being at greater risk or is there a graded association?
(b) Does network size predict illness susceptibility and, if so is its relation to illness independent of social diversity?
(c) Is having a diverse network correlated with the experience of stressful events, and do the possible beneficial effects of diverse networks only occur in the presence of stressful events?
(d) How does network diversity get "inside the body"? That is, if network diversity is associated with host resistance, does this occur because those with diverse networks have better health practices, lower levels of hormones that suppress immunity, or more effective immune response?
(e) If network diversity is associated with host resistance, can this be attributed to (spurious) personality characteristics that influence both the development and maintenance of a diverse network and host resistance to the infectious agent?
Method
Procedures
This study was carried out in Pittsburgh, PA between 1993 and 1996. Descriptions of the methods used have been published elsewhere (Cohen, Doyle, Skoner, Rabin & Gwaltney, 1997; Cohen, Frank, Doyle, Skoner, Rabin & Gwaltney, 1998). Briefly, 276 adults (125 men and 151 women) between the ages of 18 and 55 participated in the study. All volunteers initially came to the hospital for medical eligibility screenings and all who were enrolled in the study were judged to be in good health. Social networks, select health practices (smoking, alcohol consumption, exercise, sleep quality, diet), demographic factors, body weight and height were also assessed at the screening and used as baseline data for those who were found to be eligible. All eligible subjects provided informed consent approved by the Institutional Review Boards of Carnegie Mellon University, the University of Pittsburgh, and Children’s Hospital of Pittsburgh.
Eligible subjects returned to the hospital both four and five weeks after screening to have blood drawn for assessment of a marker of immune function--natural killer cell activity—that was based on both blood draws, and antibody to the experimental virus based on the second blood draw. A personality questionnaire was administered twice, once at each blood draw. Volunteers returned during the period after initial screening but before being exposed to the virus and completed an intensive stressful life events interview.
Subjects were quarantined within one week following the second blood draw. Baseline assessment of self-reported respiratory symptoms and two objective indicators of illness (nasal mucociliary clearance, and nasal mucus production) were measured during the first 24 hours of quarantine (before viral exposure). Urine samples for the assessment of cortisol, epinephrine, and norepinephrine were also collected at this time. At the end of the first 24 hours of quarantine, volunteers were given nasal drops containing a low infectious dose of one of two types of rhinovirus (RV39 [N=147] or Hanks [N=129]). Rhinoviruses are a common cause of upper respiratory (common cold) illnesses. The quarantine continued for five days after exposure. During this period volunteers were housed individually, but were allowed to interact with each other at a distance of 3 feet or more. Nasal secretion samples for verifying infection by virus culture were collected on each of the five days. On each day, volunteers completed a respiratory symptom questionnaire and were tested for objective markers of illness using the same procedures used at baseline. Approximately 28 days after challenge, another blood sample was collected for verifying infection by determination of changes in antibody to the challenge virus. All investigators were blinded to subjects' status on social network, personality, endocrine, health practice, immune, and pre-challenge antibody measures.
Social network diversity was assessed by questionnaire. The Social Network Index assesses participation in twelve types of social relationships (Cohen et al., 1997). These include relationships with a spouse, parents, parents-in-law, children, other close family members, close neighbors, friends, workmates, schoolmates, fellow volunteers (e.g., charity or community work), members of groups without religious affiliations (e.g., social, recreational, professional), and members of religious groups. One point is assigned for each kind of relationship (possible score of 12) for which respondents indicate that they speak (in person or on the phone) to someone in that relationship at least once every two weeks. The total number of persons with whom they speak at least once every two weeks (number of network members) was also assessed. [The Social Network Index and detailed scoring information are available on www.psy.cmu.edu/~scohen/ click on scales and then on Social Network Index.]
Clinical colds
Infectious diseases result from the growth and action of microorganisms or parasites in the body (see Cohen & Williamson, 1991). Infection is the multiplication of an invading microorganism. Clinical disease occurs when infection is followed by the development of symptomatology characteristic of the disease.
Biological verification of infection can be accomplished by establishing that an infectious agent is present or replicating in tissue, fluid, or both. We use two common procedures for detecting replication of a specific virus. In the viral isolation procedure, nasal secretions are cultured (put in a medium that stimulates virus replication). If the virus is present in nasal secretions, it will grow in the medium and can be detected. Alternatively, we can indirectly assess the presence of a replicating virus by looking at changes in serum antibody levels to that virus. Antibodies are protein molecules that attach themselves to invading microorganisms and mark them for destruction or prevent them from infecting cells. An invading microorganism (i.e., infection) triggers the immune system to produce antibody. Because each antibody recognizes only a single type of microorganism, the production of antibody to a specific infectious agent is evidence for the presence and activity of that agent.
Volunteers were considered to have a cold if they were both infected and met illness criteria. They were classified as infected if the challenge virus was isolated on any of the five post-challenge study days or there was a substantial rise (4-fold increase) in serum antibody level to the experimental virus. The illness criterion was based on selected objective indicators of illness--the amount of mucus produced during quarantine and mucociliary clearance function. By basing the definition of illness entirely on objective indicators, we are able to exclude interpretations of our data based on psychological influences on symptom reporting. Mucus weights were determined by collecting used tissues in sealed plastic bags. After correcting for the weight of the bag and the mucus weight at baseline, the post-challenge weights were summed across the five days to create the adjusted total mucus weight score. Nasal mucociliary clearance function refers to the effectiveness of nasal cilia in clearing mucus from the nasal passage toward the throat. Clearance function was assessed as the time required for a dye administered into the nose to reach the throat. Each daily time was adjusted for baseline and the adjusted average time in minutes was calculated across the post-challenge days of the trial. To meet clinical illness criteria, subjects had to have a total adjusted mucus weight of at least 10 grams or an adjusted average mucociliary nasal clearance time of at least 7 minutes.
Standard control variables
Standard control variables were used to examine alternative explanations for any relationship between psychosocial factors and illness. These included age, gender, ethnicity, education, body mass index (weight in kilograms divided by the square of height in meters), season during which the trial was conducted, type of experimental virus, and pre-challenge antibody titers to the experimental virus.
Statistical analyses
We used odds ratios to estimate relative risk of developing a cold. An odds ratio approximates the odds that the disease outcome (common cold) will occur in one group as compared to another. All odds ratios we report are adjusted for the standard control variables. [Standard controls are entered (forced) in the first step of a logistic regression equation, and social diversity in the second]. In each case, we report the corresponding 95% confidence intervals (CI(95%)).
Results
Social networks and susceptibility
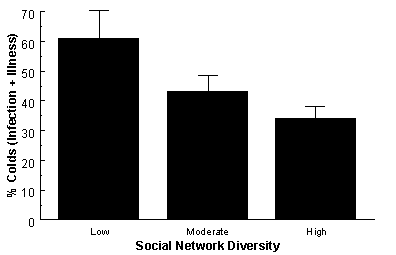
Figure 1 presents the rate of colds as a function of social network diversity. These are observed rates and are not adjusted for the standard controls. As is apparent, the rate of colds decreased as social network diversity increased. The adjusted odds ratios were 4.2 [CI (95%)=1.34,13.29] for Low Diversity, 1.9 [CI (95%)=1.00,3.51] for Moderate Diversity, and 1 for High Diversity. There were no interactions between the standard control variables and social network diversity in predicting colds. That is, the relations were similar for the two virus types, for different pre-exposure antibody levels, across seasons, and across categories of age, gender, race, education, and body mass.
Figure 1. Percentage of volunteers developing clinical colds by the diversity (# of social roles) of their social networks. Low=1-3 social roles, Moderate=4-5, and High=6 or more. Standard errors are indicated. Adapted from figure appearing in the Journal of the American Medical Association, 1997, 277, 1940-1944.
The association between total number of network members and
colds was only marginal with greater numbers associated with less
probability of developing a cold (P<.12). However, entering number
of network members into the first step of the regression equation along
with standard controls did not reduce the association between diversity
and colds (P<.01). Hence the diversity of the network is more
important than the number of network members and its association with
colds is independent of the number of members.
Stress-buffering effects of social participation
In analyses reported elsewhere (Cohen et al., 1998), we found that persons experiencing a chronic/enduring (one month or longer) stressful event as assessed by the LEDS interview were at greater risk for developing colds than those not experiencing such a stressful event. We also examined whether social participation could protect volunteers from the effects of chronic stress on illness susceptibility. First, greater numbers of social roles were not associated with fewer chronic stressful events (P=.22). Moreover, adding the chronic stressor variable to the regression equation only slightly reduced the association between network diversity and the incidence of colds (ORs = 3.9 CI(95%)=1.25, 12.23; 1.8 CI(95%)=.94, 3.35; 1.0). The interaction between network diversity and chronic stress also did not achieve statistical significance, indicating that social network diversity had the same impact on cold susceptibility for both those with and without a chronic stressor.
Pathways linking social networks to susceptibility
Those with low levels of social participation were more likely to be smokers and less likely to exercise (Cohen et al., 1997). Both of these health practices were also associated with susceptibility to colds, with smokers and those getting less exercise at greater risk. However, these health practices could explain only a small fraction of the relation between network diversity and susceptibility to infectious illness. Although higher levels of epinephrine and norepinephrine were associated with greater risk for developing a cold, neither of these hormones (or cortisol) was associated with the social network index. Hence, neither could operate as pathways linking network diversity to illness susceptibility. Also, our measure of immune function, natural killer cell cytotoxicity, was not associated with either network diversity or cold risk.
Personality as an alternative explanation
The "Big Five" personality factors are thought to represent the basic structure of personality (e.g., Goldberg, 1992). The factors are commonly described as introversion-extraversion, agreeableness, conscientiousness, emotional stability, and openness. We found that only introversion-extraversion was associated with susceptibility to colds. Those with scores below the median ("introverts") were at greater risk (adjusted OR=2.7, CI=1.45,4.92). Introversion was also associated with lower levels of social network diversity (p<.002). However, the relation between network diversity and colds occurred above and beyond (independent of) the association of introversion and colds.
Discussion
This study demonstrated that social isolation constitutes a major risk factor for the development of illness. Volunteers who were relatively socially isolated (1-3 relationships) were 4.2 times more likely to develop illness than those with very diverse networks (6 or more relationships). Although relative isolation (1-3 relationships) accounted for most of the effect, the association was graded with persons with moderate numbers of social roles (4-5) receiving some benefit. Interestingly, it was the diversity of participants’ social networks, rather than the total number of relationships they had, that predicted susceptibility. This suggests that it is something about occupying a variety of social roles (e.g., spouse, parent, co-worker, and friend) that promotes resistance to infection. How this occurs is not clear, although the present study suggests that it is not likely to be through a stress-buffering mechanism. First, the association of social network diversity and illness susceptibility was independent of the increased risk for colds found among those experiencing chronic stressful events. Second, we found no evidence for an interaction between social participation and chronic stress in predicting cold susceptibility. That is, the presence of an enduring stressor increased illness risk for volunteers across the spectrum of social network diversity.
We found that the relation between network diversity and susceptibility to the common cold was independent of network size. However, we cannot be sure that this relation is independent of other network features that might correlate with diversity, such as network density, weak ties, and structural holes (see discussion in Brissette et al., 2000). In the case of density, there is some evidence that low density social networks are associated with better mental health (Hirsch, 1980; 1981). Moreover, data we recently collected in another sample indicated that higher network diversity (as measured by the SNI) was moderately correlated with lower levels of network density, r = -.32. Weak ties—ties that connect one to networks in which one is not currently a member-- have been found to be important for tasks such as job search (Granovetter, 1973) and people who occupy structural holes—positions in networks that bridge loosely connected domains—possess greater power and status as a result of their position (Burt et al, 1997). Both concepts should covary with diversity and both have known effects that could contribute to health status and maintenance. Unfortunately, there are no existing data on the association between these concepts and network diversity, nor any evidence in regard to whether these concepts have implications for health. However, further work in this area can only give us a better understanding of how networks influence our health.
What can account for the relations between social participation, and susceptibility to infectious illness? Earlier, we raised the possibility that this association might be mediated by effects of social diversity on either health practices or on the function of the endocrine and immune systems. People with diverse social networks are thought to be subject to more social controls and engage in improved health practices (Cohen, 1988). In addition, possessing a diverse social network is thought to promote emotional regulation and influence the circulating levels of hormones capable of altering immune function. However, when we measured these potential pathways, none could account for the relations we found.
In the case of health practices, all five of the measures operated as risk factors for illness. Smokers, those abstaining from alcohol, those with poor sleep efficiency, and those with few days of exercise were at greater risk for developing colds (Cohen et al., 1997). However, health practices could account for only a small part of the relations between the social environment and host resistance. Because the health practice measures were all related to susceptibility in the expected manner, we are confident in the accuracy of our assessments. As a consequence, it seems unlikely that these health practices play a major role in linking social environments to resistance to infectious illness. Although we assessed the health practices that we thought would be most likely to provide a pathway, it is possible that other practices such as caffeine intake, use of mouth wash, or regular hand washing, might link social participation to illness susceptibility.
Those individuals with elevated levels of circulating epinephrine and norepinephrine were at greater risks for developing colds. Again, however, levels of these hormones did not provide any additional explanation of the relation between social diversity and colds. To our surprise, these hormones were not associated with the social participation measures. Because epinephrine and norepinephrine were assessed during the 24-hours before viral exposure, they might have been indicating a stress type reaction to the beginning of quarantine rather than a basal level of response to volunteers’ background environments. In our current work, we are attempting to get better background levels by measuring hormones several times during the weeks before volunteers report for quarantine. This is a case where obtaining reliable measurements (multiple measures) at appropriate points in time is essential.
We chose natural killer cell activity as our primary marker of immune function for two reasons. First, natural killer cells are surveillance cells that identify infected (and otherwise altered) cells and kill them. In theory, higher levels of natural killer cell activity should help limit infection and hence prevent illness. Second, there is evidence that chronic psychological stress is associated with suppression of NK activity (reviewed in Herbert & Cohen, 1993). However, NK activity did not operate as a pathway linking stress or social participation to illness susceptibility in our study. Measuring selected aspects of immunity in peripheral blood is not always the most appropriate procedure and may be the problem here (Cohen & Herbert, 1996). In theory, NK activity in the respiratory track might be a protective mechanism against respiratory infections. It is also possible the NK activity in the blood might make a difference, but that the ability of the immune system to compensate for deficits in single subsystems obscures any relation. At any rate, we found no evidence for immune mediation of the relations between stress and infectious illness or social participation and infectious disease. Again, we think that this may be attributable to problems in measurement.
In sum, our data are consistent with theories suggesting that occupying diverse social roles is beneficial to health. The data also support the notion that the more roles one holds the better (Marks, 1977; Sieber, 1974; Thoits, 1983), although the costs of being isolated are greater than one would expect from a purely graded relationship. Although we have proposed a number of plausible explanations of how our how a structural component of our social networks gets inside our bodies (Cohen, 1988; Cohen, Gottlieb & Underwood, 2000), the current empirical evidence does not support any specific pathway.
Using Social Network Analysis in Studies of Health
The social network measures used in studies of health outcomes probably appear rather primitive compared to those involved in formal social network analysis (readers of this journal). A primary reason that relatively simple measures are used is that studies of health outcomes typically involve large samples and include multiple questionnaires or interview measures, pushing the envelope in respect to demands on subjects. For these types of studies, concise instruments are at a premium and intensive measurement is reserved for the rare cases in which the investigator is convinced that the time is worth the potential payoff. Even so, the consistent demonstrated importance of social integration measures in health may generate a greater interest in using more elaborate quantitative measurement of social networks for these types of studies. Quantitative approaches would be especially helpful to the extent that they can be used to distinguish between alternative theories of how social integration influences health.
References
Brissette, I. Cohen, S., & Seeman, T. E. (2000). Measuring social integration and social networks. In S. Cohen, L. Underwood & B. Gottlieb (Eds.), Support measurements and interventions: A guide for social and health scientists. NY: Oxford Press.
Berkman, L. F. (1995). The role of social relations in health promotion. Psychosomatic Medicine, 57, 245-254.
Burt, R. S., Jannotta, J. E., & Mahoney, J. T. (1998). Personality correlates of structural holes. Social Networks, 20, 63-87.
Cohen, S. (1988). Psychosocial models of the role of social support in the etiology of physical disease. Health Psychology, 7, 269-297.
Cohen, S., Doyle, W. J., Skoner, D. P., Rabin, B. S. & Gwaltney, J. M. (1997). Social ties and susceptibility to the common cold. Journal of the American Medical Association, 277, 1940-1944.
Cohen, S., Frank, E., Doyle, B. J., Skoner, D. P., Rabin, B. S. & Gwaltney, J. M. (1998). Types of stressors that increase susceptibility to the common cold. Health Psychology, 17, 214-223.
Cohen, S., Gottlieb, B., & Underwood, L. (2000). Social relationships and health. In S. Cohen, L. Underwood, & B. Gottlieb (eds.), Measuring and intervening in social support. New York: Oxford Press.
Cohen, S. & Herbert, T. A. (1996). Health psychology: Psychological factors and physical disease from the perspective of human psychonueroimmunology. Annual Review of Psychology, 47, 113-142.
Cohen, S., & Williamson, G. (1991). Stress and infectious disease in humans. Psychological Bulletin, 109, 5-24.
Cohen, S., & Wills, T. A. (1985). Stress, social support and the buffering hypothesis. Psychological Bulletin, 98, 310-357.
Coser, L. (1974). Greedy Institutions. New York, NY: Free Press.
Durkheim, E. (1896/1951). Suicide. New York, NY: Free Press.
Faris, R. E. L. (1934). Cultural isolation and the schizophrenic personality. American Journal of Sociology, 40, 155-169.
Glaser, R., Rabin, B., Chesney, M., Cohen, S., & Natelson, B. (1999). Stress-induced immunomodulation: Implication for infectious disease? Journal of the American Medical Association, 281, 2268-2270.
Goldberg, L. R.. (1992). The development of markers for the Big-Five factor structure. Psychological Assessment,4, 26-42.
Goode, W. J. (1960). A theory of role strain. American Sociological Review, 25, 483-496.
Granovetter, M. (1973). The strength of weak ties. American Journal of Sociology, 81, 1287-1303.
Helgeson, V. S., Cohen, S., & Fritz, H. L. (1998). Social ties and the onset and progression of cancer. In J. Holland (Ed.), Textbook of Psycho-oncology.
Herbert, T. B., & Cohen, S. (1993). Depression and immunity: A meta-analytic review. Psychological Bulletin, 113, 472-486
Hirsch, B. J. (1980). Natural support systems and coping with major life events. American Journal of Community Psychology, 8, 159-172.
Hirsch, B. J. (1981). Coping and adaptation in high risk populations: Toward an integrative model. Schizophrenia Bulletin, 7, 164-172.
House, J. S., Landis, K. R., & Umberson, D. (1988). Social relationships and health. Science, 241, 540-545.
Jaco, E. (1954). The social isolation hypothesis and schizophrenia. American Sociological Review, 19, 567-577.
Marks, S. (1977). Multiple roles and role strain: Some notes on human energy, time, and commitment. American Sociological Review, 42, 921-936.
Mead, G. H. (1934). Mind, Self, and Society. Chicago: University of Chicago Press.
Orth-Gomer, K. & Johnson, J. V. (1987). Social network interaction and mortality: A six year follow-up study of a random sample of the Swedish population. Journal of Chronic Disease, 40, 949-957.
Rabin, B. S. (1999). Stress, immune function and health: The connection. New York: John Wiley & Sons.
Rook, K. S. (1990). Social networks as a source of social control in older adults’ lives. In H. Giles, N. Coupland, & J. Wiemann (Eds.) Communication, health and the elderly (pp. 45-63). Manchester, England: University of Manchester Press.
Sieber, S. D. (1974). Toward a theory of role accumulation. American Sociological Review, 39, 567-578.
Slater, P. (1963). On social regression. American Sociological Review, 28, 339-364.
Stryker, S. (1980). Symbolic interactionism: A social structural version. Menlo Park: Benjamin/Cummings.
Thoits, P. A. (1983). Multiple identities and psychological well-being: A reformulation of the social isolation hypothesis. American Sociological Review, 48, 174-187.
Umberson, D. (1987). Family status and health behaviors: Social control as a dimension of social integration. Journal of Health and Social Behavior, 28, 306-319.
Ware, E. H. (1956). Mental illness and social conditions in Bristol. Journal of Mental Science, 102, 349-357.